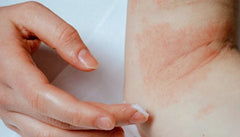
300+ clinicians, doctors, and dermatologists have shared Svens Island for eczema relief, with no compensation.
You've tried the steroids, the prescriptions, the thick moisturisers that promised relief.
For a few days, maybe even a week, things improved. The redness softened. The itch eased. You finally slept properly.
And then it came back.
If this has been your experience, you are not alone and you’re not doing anything wrong.
The cycle of flare, treat, calm, repeat is one of the most common frustrations for people managing eczema. Understanding why it happens is usually the first step to changing it.
The Short Answer
Eczema keeps coming back because most treatments only address what is visible. Two issues are usually still active beneath the surface, even when the skin looks calm:
-
A weakened skin barrier that has not fully recovered
-
Bacterial imbalance that keeps the inflammatory cycle going
When the barrier is compromised, moisture escapes and irritants get in more easily.
The skin becomes dry, reactive, and quick to inflame – creating the ideal conditions for a bacterium called Staphylococcus aureus to multiply.
This bacterium makes inflammation worse and harder to resolve.
Steroids can calm that inflammation quickly. But they do not repair the barrier or reduce Staph. When you stop using them, both problems are still there.
That’s why relief feels temporary – why you stay stuck in the flare cycle. 
Eczema Is Not Just Dry Skin
Most people are told eczema is dry, sensitive skin. Moisturise it. Manage it. Avoid triggers.
But there’s often a deeper structural issue that this explanation misses.
The outermost layer of your skin is designed to act like a seal. It holds moisture in and keeps irritants, microbes, and environmental stress out.
In eczema-prone skin, that seal is structurally weaker – often due to genetics outside of your control.
Tiny gaps form between skin cells. Natural moisturising factors are reduced. The lipids that hold the barrier together become less stable.
The result of a weaker barrier is skin that loses water faster, is more sensitive to triggers, and inflames more easily.
Even between flares, eczema-prone skin is working harder than healthy skin just to stay calm. When the barrier has not properly recovered, it does not take much to start the next flare.
The Inflammation Loop
Once the barrier weakens, the immune system begins overreacting to things it would normally tolerate. Dust. A change in temperature. A new laundry detergent. These become triggers.
That overreaction creates inflammation. Inflammation drives itch. Itch leads to scratching. Scratching damages the barrier further.
That loop alone can sustain recurring eczema. But there is another layer that often explains why some flares feel particularly hard to resolve.
How Bacteria Makes Flares Worse
When skin is inflamed and the barrier is compromised, the surface environment shifts. Staphylococcus aureus - a key driver of eczema - finds it much easier to colonise and multiply.
The more inflamed the skin, the more easily Staph takes hold. The more Staph takes hold, the harder it is for inflammation to settle.
Staph releases substances that intensify the immune response, disrupt barrier repair, and amplify itching. The sequence tends to look like this:
-
Barrier damage makes the skin easier to inflame
-
Inflamed skin creates conditions where Staph thrives
-
Staph aggravates the inflammation further
-
That drives more scratching
-
Which worsens barrier damage
That's the endless loop of flare, temporary calm, then flare again.
Without addressing both barrier integrity and bacterial balance, this loop can continue even when the skin appears to be settling. Which is why the next flare often arrives sooner than expected.
What the Research Says About Staph Bacteria, Weakened Skin Barriers and Genetics
The connection between skin barrier dysfunction, bacterial imbalance, and recurring eczema is well-established in dermatology.
Many people with eczema carry genetic variations that reduce a structural protein called filaggrin. Without sufficient filaggrin, the barrier develops gaps - moisture escapes more readily and irritants penetrate more easily.
This is part of why eczema-prone skin is often reactive even between flares, not just during them.¹
During active flares, Staphylococcus aureus is present on the skin of up to 90% of people with eczema², compared to around 5% of people who don’t have eczema.² Its role in sustaining and worsening flares is consistently supported by research.
Repeated inflammation and scratching also cause cumulative changes over time - thickening in some areas, thinning in others - which can lower the threshold for future flares if the underlying cycle is not addressed.³
Research published in the Journal of Allergy and Clinical Immunology shows that when bacterial balance is restored alongside barrier support, disease severity decreases and flares become less frequent.⁴
The two are connected. Addressing one without the other usually means the cycle just keeps going.
Why Flares Can Feel Worse Over Time
When the inflammatory cycle repeats frequently, the skin can become progressively more reactive. Repeated flares may contribute to:
-
Thickened skin in areas of chronic scratching
-
Thinner, more fragile patches elsewhere
-
Heightened nerve sensitivity
-
A lower threshold for what triggers itch
This is not irreversible. But it does mean the skin benefits from sustained, consistent support - not just treatment when things get bad.
Stopping a routine as soon as the skin calms is one of the most common reasons the cycle continues.
Common Mistakes That Keep Eczema Returning
Most people with eczema have fallen into at least one of these patterns. They are understandable and genuinely hard to avoid.
-
Stopping treatment as soon as the flare clears. The skin looks better, so you stop applying treatments. But the barrier is still fragile and bacterial balance is still off. Stopping at this point leaves the skin in essentially the same state that allowed the last flare to begin.
-
Only treating during flares, not between them. Reactive care matters, but it is not sufficient on its own. Consistent daily support between flares is what gives the barrier a real chance to recover. Think of it less like treating a wound and more like maintaining a defence.
-
Using products that further compromise the barrier. Fragranced soaps, harsh washes, and some medicated cleansers disrupt the skin's natural pH and damage the barrier while trying to address other symptoms. For eczema-prone skin, gentle and pH-balanced is not optional.
-
Expecting linear progress. Eczema management rarely follows a straight line. Two steps forward, one step back is common, especially in the early weeks of a new routine. Giving up before the barrier has had adequate time to rebuild is one of the most frequent reasons people feel stuck.
Setting Realistic Expectations
Rebuilding the skin barrier takes time. It cannot be rushed.
Most people notice improvement in stages:
-
First, the itch becomes less intense
-
Then the skin feels more settled and redness softens
-
Then sleep improves
-
Then gaps between flares grow longer
This progression typically takes days to weeks, sometimes longer. Staying consistent is essential. The goal is calmer, more resilient skin over time - not perfect skin within days.
Understanding this from the start makes a real difference. Most people abandon routines just before they would have started to see results.
A Barrier-First, Bacteria-Aware Approach
To interrupt the inflammation cycle, the shift is usually from reactively treating new flares to consistent prevention.
That means focusing on daily barrier support, gentle cleansing that does not strip protective lipids, and ingredients that help maintain bacterial balance without aggressive disruption. It means building a routine gentle enough to use every day - not just when things get bad.
The other shift is in expectation. Results from this kind of approach are not immediate. But they compound. Skin that is consistently supported becomes more resilient over time, and that resilience is what reduces how often and how severely flares return.
Certain botanical ingredients - like Manuka leaf oil, Marshmallow Root and Coconut Oil - have been studied for their antimicrobial and skin-supportive properties. For those looking for a steroid-free approach that addresses both barrier repair and bacterial balance, Sven's Island Miracle Manuka Creme is one option worth exploring.
Frequently Asked Questions
Is eczema caused by bacteria?
No. Eczema is a complex inflammatory condition involving genetics, immune function, and barrier dysfunction. However, bacterial imbalance - particularly elevated Staphylococcus aureus during flares - is strongly associated with symptom severity and how long flares last.
Why do flares come back worse after stopping steroids?
Steroid creams work fast - but they treat the symptom, not the cause. The barrier damage and bacterial imbalance that drove the original flare are still present. When you stop, the skin is just as vulnerable as before, and for many people the inflammation returns harder. This is called steroid rebound, and it is one of the more disheartening parts of managing eczema long term.
How long does it take to strengthen the skin barrier?
Meaningful improvement often begins within two to four weeks of consistent care. Full resilience takes longer depending on severity. Skin cell turnover occurs roughly every 28 days, so structural change is gradual. Many people notice comfort improvements - reduced itch, better sleep - before that point.
What triggers eczema recurrence?
Dry air, stress, allergens, sweat, and irritants like fragranced soaps are common. Bacterial imbalance on the skin surface can also restart the cycle, particularly after the barrier has recently been compromised.
Should I avoid steroids completely?
Not necessarily. Steroids have a legitimate role in managing acute flares under medical guidance. What many people find helpful is building a consistent barrier-first routine alongside medical care, so that over time they need to rely on steroids less - not as a replacement, but as part of a more complete approach.
Final Thought
If your eczema keeps coming back, it is not random.
It reflects an ongoing cycle - barrier vulnerability, inflammation, bacterial imbalance - that short-term treatment alone rarely addresses fully.
Breaking that cycle takes consistent barrier support, realistic expectations, and patience. Progress is not dramatic at first. But over months of steady care, the skin becomes more resilient. Flares become less frequent and less severe.
That is the difference between constantly managing eczema and genuinely getting ahead of it.
References
¹ Genetic variations weakening barrier: Gupta et al. (2020).
² Staph overgrowth on lesional skin (90%): Biedermann (2008), NEJM.
³ Repeated inflammation/scratching thinning skin: Mayo Clinic.
Don’t Miss These
Works well with Eczema prone skin
- $66.00
-
$104.00 - $66.00
- -37%
- Unit price
- per
- $62.00
-
$89.00 - $62.00
- -30%
- Unit price
- per
- $99.00
-
$145.00 - $99.00
- -32%
- Unit price
- per
- $40.00
-
- $40.00
- -0%
- Unit price
- per