300+ clinicians, doctors, and dermatologists have shared Svens Island for eczema relief, with no compensation.
The skin of most people with eczema carries elevated levels of Staphylococcus aureus (Staph bacteria) at all times. This is colonisation – bacteria living on the skin surface – and it plays a significant role in driving inflammation and flare cycles.
But colonisation is not the same as infection. True infection happens when Staph penetrates through broken skin into deeper tissue layers, triggering a response that's harder to manage and potentially more serious.
Understanding where the line is – and what it looks like – is key for anyone managing eczema to know.
The Difference Between Colonisation and Infection
Around 90% of people with eczema have Staph on their skin during flares, compared to 5-30% of people without eczema. That elevated colonisation contributes to the itch-scratch cycle even when there's no visible sign of infection. It's part of why flares are hard to break and why skin barrier repair and bacterial balance matter so much in daily management.
True bacterial infection is different. It occurs when bacteria – most commonly Staph, occasionally Group A Streptococcus – breach the skin barrier and invade deeper layers. This triggers a more intense immune response, produces specific visible symptoms, and in some cases requires antibiotic treatment rather than topical management alone.
The key distinction is depth. Colonisation sits on the surface. Infection has gone through it.
What a Bacterial Infection Looks Like
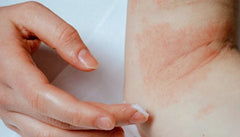
Bacterial infection on eczema-prone skin has recognisable visual signs that distinguish it from a standard flare. Knowing what to look for means you can act earlier – and avoid the progression from manageable infection to something more serious.
Honey-coloured crusting. This is the most classic sign of impetiginized eczema – eczema with a secondary bacterial infection. A golden or amber crust forming over a patch is a reliable indicator that Staph has moved from surface colonisation into infection territory.
Yellow or white pus. Weeping or discharge from eczema patches that is yellow or white rather than clear suggests bacterial activity beyond normal inflammation. Clear weeping can happen with severe eczema alone – coloured discharge is a stronger warning sign.
Pustules or blisters. Small pus-filled spots or blisters appearing on top of or around eczema patches indicate bacterial involvement. These are distinct from the dry, cracked, or weeping appearance of standard eczema.
Boils or folliculitis. Pus-filled bumps around hair follicles – folliculitis – or larger boils developing near eczema patches suggest Staph is spreading beyond the original affected area.
Swelling and warmth. Skin around an eczema patch that becomes noticeably swollen, warm to the touch, and tender – particularly if the area is expanding – can indicate cellulitis, a deeper skin infection that requires prompt medical attention.
"Tangerine glisten." Before crusting develops, some eczema-affected skin takes on a subtle orange or amber sheen – sometimes described as a tangerine glisten. This early sign often precedes visible crusting and is worth noting if it appears.
Sensation Changes That Signal Infection
The sensation of an infected patch is different from a standard flare – and these changes are often what prompts people to seek help.
Pain rather than itch. Standard eczema produces itch. Bacterial infection produces pain – a distinctly different sensation that doesn't respond to scratching or antihistamines the way itch does.
Burning. A new burning sensation over an eczema patch, particularly if it wasn't present before, is a consistent early sign of bacterial infection.
Tenderness to touch. Skin that's tender or painful when pressed – rather than just itchy - suggests inflammation has gone deeper than the surface.
When to Seek Medical Care Immediately
Some signs indicate the infection has moved beyond the skin surface and requires prompt medical attention.
Fever or chills. Any fever accompanying a skin flare suggests the infection may be entering the bloodstream. This requires same-day medical assessment.
Feeling generally unwell. Malaise, fatigue, or feeling systemically unwell alongside worsening skin is a sign the body is responding to something beyond localised inflammation.
Rapid spreading. An infected area that's visibly expanding – particularly with increasing warmth and swelling - can indicate cellulitis. Left untreated, cellulitis can progress to more serious systemic infection.
If any of these systemic signs are present, see a doctor the same day rather than managing at home.
Why Eczema Skin Is Particularly Vulnerable
The progression from colonisation to infection follows a predictable path in eczema-prone skin. A compromised barrier allows Staph to access deeper skin layers. Infection triggers more inflammation. Inflammation drives scratching. Scratching opens bigger gaps in the barrier. More Staph enters.
This cycle can escalate from increased redness and itch on days one and two, to weeping, crusting, and pustules by days three and four, to pain, swelling, and possible fever by day five and beyond. Catching it at the early visual stage – honey crusting, pustules – gives the most options for management and the best chance of avoiding systemic involvement.
The face, elbows, and knees are the most common sites for infection in eczema-prone skin – areas where the barrier tends to be most compromised and scratching is most frequent.
What the Research Shows
Research confirms most eczema skin carries Staph aureus – but distinguishes colonisation from true infection clearly. Staph aureus is present on 70-90% of eczema lesions during flares (vs 5-30% healthy skin), driving inflammation even without invasion.¹
Barrier damage predicts infection risk. Studies show higher transepidermal water loss (TEWL) and a genetic predisposition to reduced filaggrin in the skin directly correlate with Staph aureus penetration into deeper skin layers, turning colonisation into active infection.²
Honey-coloured crusting – the hallmark of impetiginized eczema – is Staph aureus infection confirmed in 85% of cases, reliably distinct from sterile eczema weeping.³
Only 10-20% of Staph aureus-colonised flares progress to true infection needing antibiotics – most respond to barrier repair + topical management.⁴
Daily emollients cut infection rates 3X by strengthening barrier function and reducing scratching that creates bacterial entry points.⁵
These patterns show why daily barrier care and bacterial balance prevents most infections before they start.
What to Do When You Suspect Infection
Mild infection (crusting only). Honey-coloured crusting without pus, swelling, or systemic symptoms can often be managed with topical antibiotics prescribed by a GP alongside consistent barrier support. Don't attempt to remove crusts – this can spread bacteria and worsen the infection.
Moderate infection (pus and swelling). Yellow discharge, pustules, or localised swelling and warmth indicate deeper bacterial involvement. Oral antibiotics are typically needed at this stage. See a doctor within 24 hours.
Severe infection (fever, cellulitis, or systemic symptoms). Any fever, rapidly spreading warmth and swelling, or feeling generally unwell requires same-day medical assessment. In severe cases, hospitalisation may be needed.
Reducing Infection Risk Long-Term
Most bacterial infections in eczema are preventable. The risk is highest when the barrier is most compromised – which is why consistent daily barrier support, not just reactive treatment during flares, is the most effective long-term strategy.
Keeping Staph levels low on the skin surface between flares reduces the bacterial load available to penetrate when the barrier is disrupted. Manuka leaf oil has been specifically studied for its ability to fight Staph, including disrupting the biofilms bacteria form on the skin surface. Used consistently as part of a daily barrier repair routine, it addresses the colonisation that precedes infection rather than waiting for infection to develop.
Sven's Island Miracle Manuka Cream is formulated for exactly this kind of consistent daily use – reducing Staph colonisation while supporting barrier repair, gentle enough for daily use from birth.
Frequently Asked Questions
How do I know if my eczema is infected?
The most reliable signs are honey-coloured crusting, yellow or white pus, pustules on or around eczema patches, and pain rather than itch. Standard eczema produces itch – infection produces pain, burning, and tenderness. If you're unsure, see a GP who can assess whether topical or oral antibiotics are needed.
Can eczema get infected without looking obviously infected?
Yes. In early stages, infection can present as increased redness and itch beyond the usual baseline, a subtle orange-amber sheen on the skin, or a flare that's not responding to standard management. These early signs often precede the more obvious visual indicators like crusting and pus.
Is weeping eczema always infected?
No. Clear weeping is common in severe eczema without infection – it's plasma from inflamed skin, not bacterial discharge. Yellow or white weeping suggests bacterial involvement and warrants medical assessment.
How quickly can eczema become infected?
The progression can be rapid – increased redness on day one or two, visible crusting or pustules by day three or four, and possible systemic symptoms by day five or beyond. Early recognition and prompt treatment at the crusting stage prevents progression to more serious infection.
Does infected eczema need antibiotics?
It depends on severity. Mild infection with crusting only can sometimes be managed with topical antibiotics. Moderate infection involving pus, swelling, or spreading warmth typically requires oral antibiotics. Severe infection with systemic symptoms requires same-day medical assessment and possibly hospitalisation.
Final Thought
Staph on eczema skin is almost universal – colonisation is part of the condition, not a sign that something has gone wrong. But when colonisation tips into infection, the signs are specific and recognisable.
Knowing what honey crusting looks like, understanding when pain replaces itch, and knowing when to seek medical care versus managing at home is what separates a managed infection from one that escalates.
And reducing the colonisation that creates infection risk in the first place – through consistent daily barrier and bacterial balance support – is what stops a flare from becoming an infection.
References
¹ Totté et al. (2016), Br J Dermatol. https://pubmed.ncbi.nlm.nih.gov/26994362/
² McAleer et al. (2024), JCI Insight. https://insight.jci.org/articles/view/178258
³ StatPearls (2024), Impetigo. https://www.ncbi.nlm.nih.gov/books/NBK430974/
⁴ Paller et al. (2019), J Allergy Clin Immunol. https://www.jacionline.org/article/S0091-6749(18)31664-6/fulltext
⁵ Hon et al. (2013), BMC Dermatol. https://pmc.ncbi.nlm.nih.gov/articles/PMC3665665/
Mentioned in this article
Works well with Eczema prone skin
- $66.00
-
$104.00 - $66.00
- -37%
- Unit price
- per
- $62.00
-
$89.00 - $62.00
- -30%
- Unit price
- per
- $99.00
-
$145.00 - $99.00
- -32%
- Unit price
- per
- $40.00
-
- $40.00
- -0%
- Unit price
- per